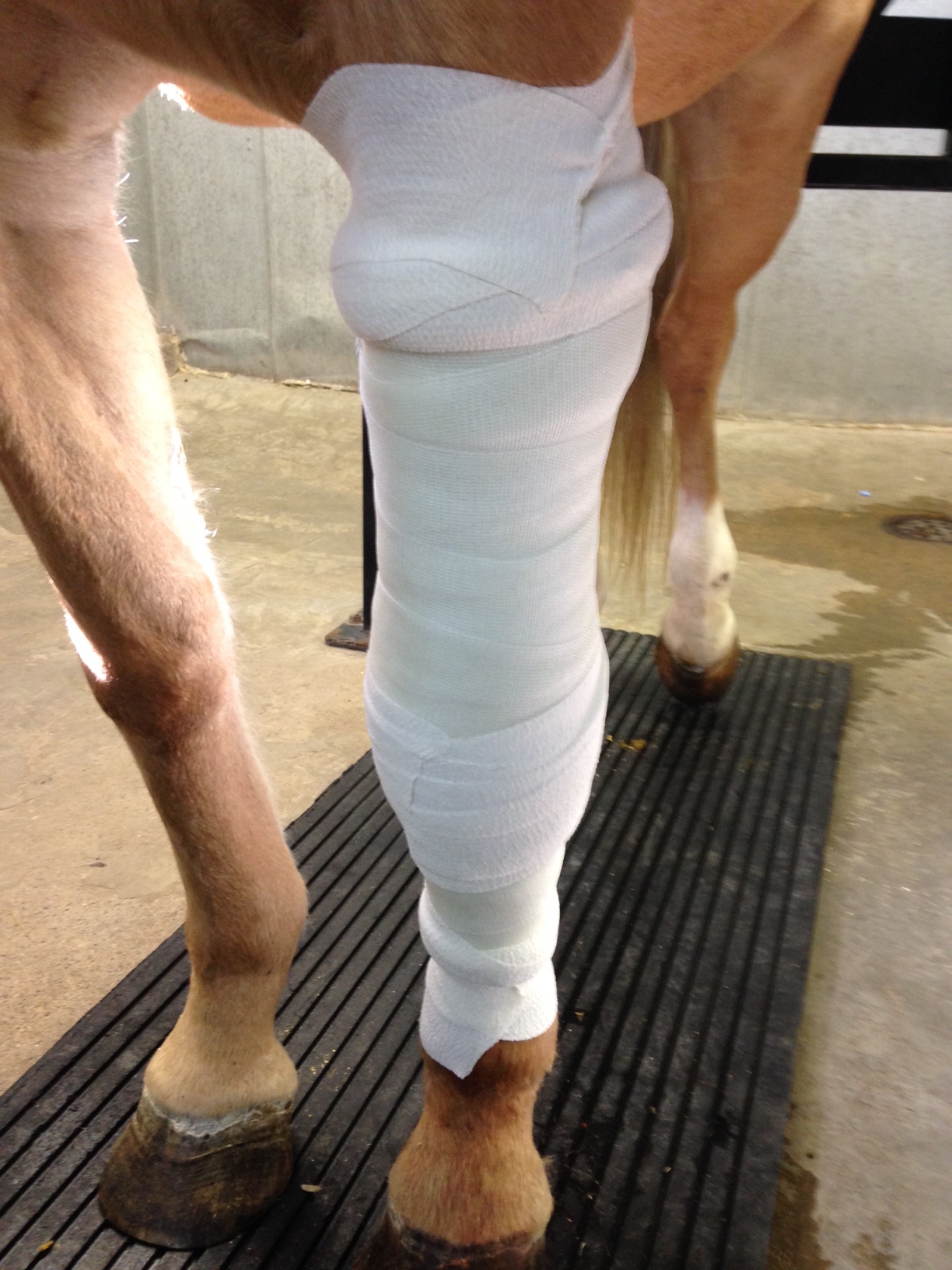
Sugar - Skin Grafting
Sugar sustained a major laceration to the front of her carpus during the big snowstorm we had in September 2014. Even though her owner found it the day it happened, there was already a large amount of swelling present as well as a large amount of dirt and contamination in the wound. Initial treatment included intravenous regional limb perfusions with antibiotics, intravenous antibiotics, and bandaging.
Although it would have been ideal to distend the carpal joints with saline to ascertain whether the laceration communicated with the joints, this wasn't possible without fear of introducing contamination into the joint given the amount of swelling. Therefore, radiographs were taken with contrast injected into the wound. These radiographs did not show any contrast inside the joint capsule, making it much less likely that the joints were involved.
Sugar had a total of five intravenous regional limb perfusions with antibiotics, and continued on systemic antibiotics and frequent bandage changes for the next month. A splint was applied to the back of the bandage to keep her limb straight. One of the main challenges of a wound in this particular area is the amount of motion - every time the horse bends its knee, the wound gapes open. This movement had to be neutralized in order for the wound to heal.
By about a month after the initial trauma, the wound had filled in with granulation tissue. At this time, we felt a skin graft would provide the quickest and best chance of healing. In horses, skin grafting is most commonly done using full thickness free island autografts transferred from one site to another on the same individual. One of the main requirements for grafting is a granulation tissue bed that is free of infection; it is necessary to prepare the wound bed to ensure the best chance of success. The purpose of island grafting is to increase the surface area of skin from which epithelialization (skin growth) can proceed, enabling the wound to heal in a timely fashion. Types of island grafts include punch grafts, pinch grafts, and tunnel grafts.
Because of the large amount of motion present on the front of the carpus, we decided to use pinch grafts in this wound. Pinch grafts are small 3mm discs of skin, harvested by removing an elevated cone of skin, that are implanted into small slits in the granulation tissue. Common inconspicuous sites from which to take the skin (the donor sites) include the portion of the neck that lies beneath the mane or underneath the abdomen. We decided to use the neck in Sugar's case. The grafts were removed in a symmetrical pattern, and the small wounds created were sutured closed.
The recipient pockets in the wound itself were actually created several hours in advance to allow the bleeding to stop before the implantation of the grafts. Once harvested, the grafts were kept on a saline-soaked gauze before they were placed into each tiny pocket in the wound, about 3-5mm apart.
Since the grafts take several days to start to attach and grow blood vessels, it is imperative that there is no motion at the grafting site. Any shearing forces between the graft and the recipient bed dislodge the fibrin seal. A cast was applied immediately after the grafts were placed, and remained in place for two days. After this, the cast was split in two, and half of the cast was used as a splint.
In any pinch grafting procedure, we expect the thin layer of granulation tissue covering each graft to slough in the first one to two weeks. Within three weeks, we hope to see epithelium (skin) start to migrate from the margin of each graft. One can expect about 50-75% of the grafts to survive.
Sugar remained in a bandage and splint for several months after the grafting procedure. The majority of the grafts survived, and with conscientious care and bandage changes the wound healed well. A scar is present with sparse tufts of hair covering it - this is typical for the cosmetic appearance of a wound that is treated with island skin grafts. Sugar has returned to her pasture, and by all accounts is glad to finally be bandage-free!